CERVICAL CANCER
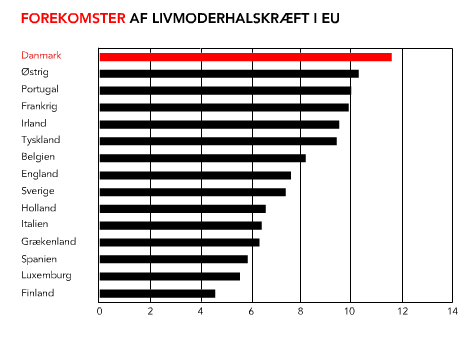
Denmark has the highest incidence and the highest mortality from cervical cancer
Cervical cancer is one of the gynaecological types of cancer. Worldwide, it is the second most common type of cancer in women with around 500,000 new cases per year. In Europe, the incidence of cervical cancer amounts to around 60,000 and the mortality to almost 30,000 every year.
Compared to all other countries in the EU, Denmark has the highest incidence and the highest mortality from cervical cancer. See the image to the right.
Cervical cancer is mainly seen in women between the age of 35 and 55, where many women have children at home and are active in the labour market, and the disease therefore leads to major social consequences. The average age at the time of diagnosis of cervical cancer is lower than is the case for many other types of cancer, and cervical cancer is therefore responsible for a large number of lost years of living.
From research over the last 10-15 years, we have gained an extensive knowledge of the primary causes of cervical cancer. For example, we now know that infection with certain types of human papilloma virus (HPV) is a prerequisite factor for cervical cancer to develop. Infections with HPV, however, are very common, and in most cases the infection
disappears again without causing any problems. For reasons not yet known, the HPV-infection becomes chronic with some women, and it is especially this chronic infection which is connected to an increased risk of cervical cancer.
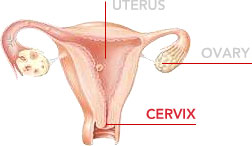 Cervical cancer is presumed to develop over many years with a number of preliminary stages of increasing degrees of severity (cellular changes). These preliminary stages or cellular changes can be detected by phrophylactic examinations (screenings) of cellular samples. Thanks to the phrophylactic examinations of cellular samples, the number of cervical cancer cases has fallen considerably over the last 40-50 years.
Cervical cancer is presumed to develop over many years with a number of preliminary stages of increasing degrees of severity (cellular changes). These preliminary stages or cellular changes can be detected by phrophylactic examinations (screenings) of cellular samples. Thanks to the phrophylactic examinations of cellular samples, the number of cervical cancer cases has fallen considerably over the last 40-50 years.
Still, more than 400 Danish women are diagnosed with cervical cancer every year, and up to 5,000 women have to go through conic section surgery because of severe cervical cellular changes.
Even in countries with efficient screening against cervical cancer, the reduction in the number of cervical cancer cases seems to have stagnated. This indicates that the limit to what can be gained by screening with cellular samples has been reached. Persistent research is being carried out to further improve the prevention of cervical cancer. The HPV testing is a promising method for the improvement of the screening. Furthermore, a vaccine against HPV has been found efficient in early clinical tests and will hopefully contribute to further reduction in cervical cancer in the future.
Read more about cervical cancer on www.cancer.dk, www.dgc-dk.dk andwww.ecce.org
Read more about Ovarian cancer Read more about Uterine cancer